Liver Transplantation: What You Need to Know Right Now
Facing a possible liver transplant is scary and confusing. You probably have a thousand questions: Do I qualify? How long do I wait? What happens after surgery? This page gives straightforward, usable answers so you can make better decisions and feel more in control.
Who needs a liver transplant?
A liver transplant is an option when the liver can’t do its job anymore. Common reasons include end-stage cirrhosis from hepatitis or alcohol, acute liver failure, and certain metabolic or cancer conditions. Doctors use scores—most commonly the MELD score—to measure how urgently someone needs a transplant. Higher MELD means higher priority on the waiting list.
Being eligible isn’t automatic. You’ll go through a full evaluation: medical tests, imaging, mental health and social support checks, and sometimes financial review. Teams look for other health problems that could complicate surgery, plus whether you have the support needed for recovery.
Types of transplants and the waiting list
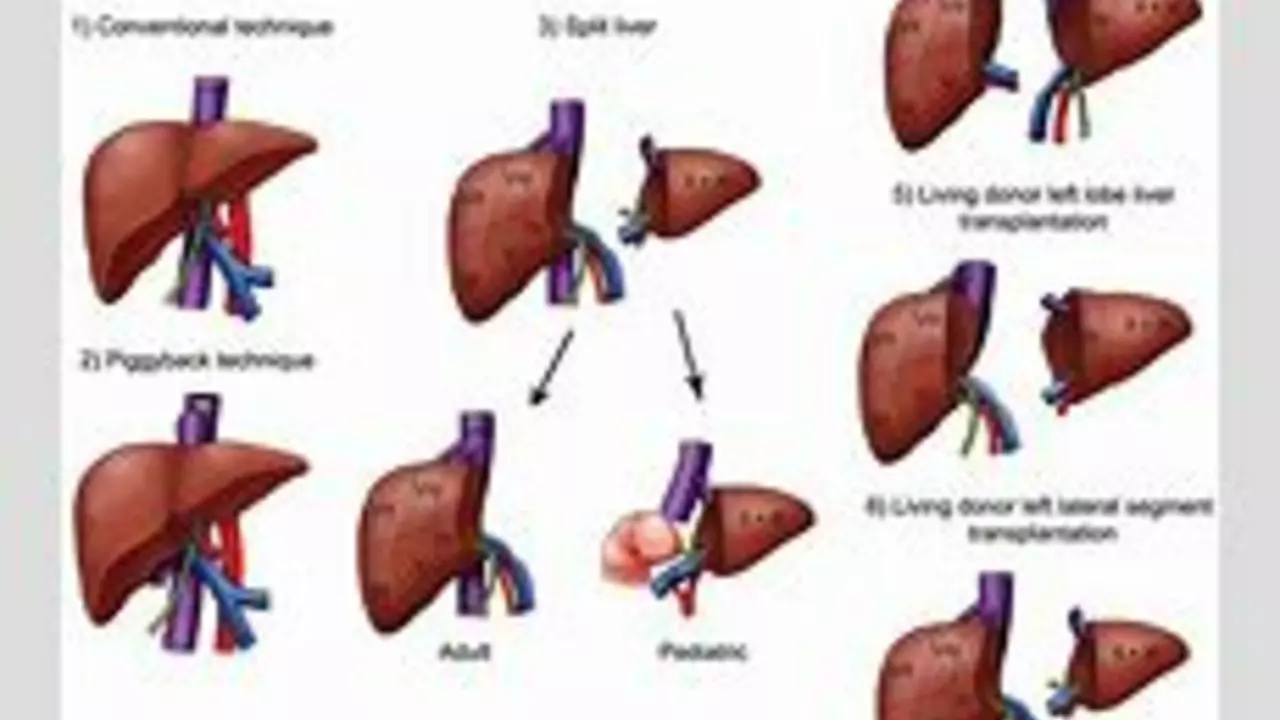
There are two main donor types: deceased donors and living donors. Deceased donor livers come from people who died and donated organs. Living donor transplants involve a person—often a family member—who gives part of their healthy liver. Living donations can shorten wait time and are a good option when available.
Wait times vary by region, blood type, and how sick you are. While on the list, you’ll get regular checkups and tests. Keep your contact info up to date and follow your team’s instructions—missing a call can cost you a chance at an organ.
Surgery usually takes several hours. Afterward you’ll stay in the hospital for days to a couple of weeks, then months of follow-up. Early recovery focuses on pain control, wound care, preventing infection, and starting immunosuppressant drugs so your body accepts the new liver.
Rejection is possible but not inevitable. Teams monitor liver function with blood tests and sometimes biopsies. If rejection shows up, medications can often control it. The goal is long-term survival with good quality of life.
Medication adherence matters. Immunosuppressants lower rejection risk but raise infection risk. You’ll need vaccinations, regular labs, and lifestyle changes—no heavy drinking, balanced diet, and safe exercise. Tell every doctor you see that you’re a transplant recipient; some meds and vaccines must be avoided or adjusted.
Practical tips: keep a transplant passport with meds and allergies, bring a list of questions to clinic visits, and build a support plan for transport and home care after surgery. Emotional support is as important as medical care—don’t hesitate to ask for counseling.
If you want more reading, talk to your transplant center and look for patient guides from major transplant organizations. SafeMeds4All is here to help you understand medicines and recovery steps so you can focus on getting better.
Hepatic Encephalopathy: The Role of Liver Transplantation in Treatment
Hepatic encephalopathy is a severe neurological disorder that can occur due to liver failure. In my recent research, I discovered that liver transplantation is considered the most effective treatment for this condition. The procedure helps in preventing further brain damage and improves the patient's overall quality of life. However, it's important to note that liver transplantation is a major surgery with potential risks and complications. Therefore, thorough evaluation and monitoring of patients is crucial for a successful outcome.
