Hepatic encephalopathy — what it is and why it matters
Hepatic encephalopathy (HE) is a brain function change that happens when the liver can’t clear toxins from the blood. Toxins like ammonia build up and affect thinking, sleep, and coordination. HE can be sudden and severe or come on slowly and be subtle. Knowing the signs and what to do can prevent a serious emergency.
Recognizing symptoms
Early signs are often mild: sleep pattern shifts, short-term memory slips, slowed thinking, or trouble doing routine tasks. Watch for more obvious changes like confusion, personality shifts, slurred speech, and a shaky flapping movement of the hands called asterixis. Severe HE can cause extreme drowsiness, unresponsiveness, or coma. If someone with liver disease becomes suddenly confused or hard to wake, they need emergency care.
Common triggers include gastrointestinal bleeding, infections, dehydration, constipation, new or increased sedatives, and electrolyte problems. Even skipping medications or eating a very high-protein meal can spark an episode in some people. Identifying and treating these triggers is as important as treating HE itself.
Treatment and practical steps
Initial treatment aims to clear toxins and fix the trigger. Lactulose is the first-line medicine. It’s given by mouth or as an enema and is adjusted so you get about two to three soft stools a day. Rifaximin, a non-absorbable antibiotic, is often added if episodes repeat despite lactulose. Doctors also look for and treat infections, stop sedatives, replace fluids, and correct low potassium or sodium.
Ammonia blood tests are commonly done, but numbers don’t always match how a person looks. Doctors use the whole clinical picture—symptoms, exam, and tests—to decide treatment. Sometimes an EEG is used if the diagnosis is unclear.
For chronic management, aim to prevent triggers: keep hydrated, treat constipation promptly, avoid alcohol and sedatives, and follow prescribed meds. While old advice pushed protein restriction, current practice supports regular protein intake—often plant or dairy sources—because staying nourished helps recovery and strength.
Practical tips: keep a simple checklist for caregivers (med list, recent bleeds or infections, bowel movements). If you use lactulose, learn the right dose and what stool changes to target. If someone with known liver disease shows any drop in alertness, don’t wait. Early treatment at home or in the ER prevents progression.
Follow-up is key. People who have had HE need regular liver care and clear plans for medication and emergency contacts. With prompt treatment and attention to triggers, many people keep HE under control and avoid repeated hospital stays.
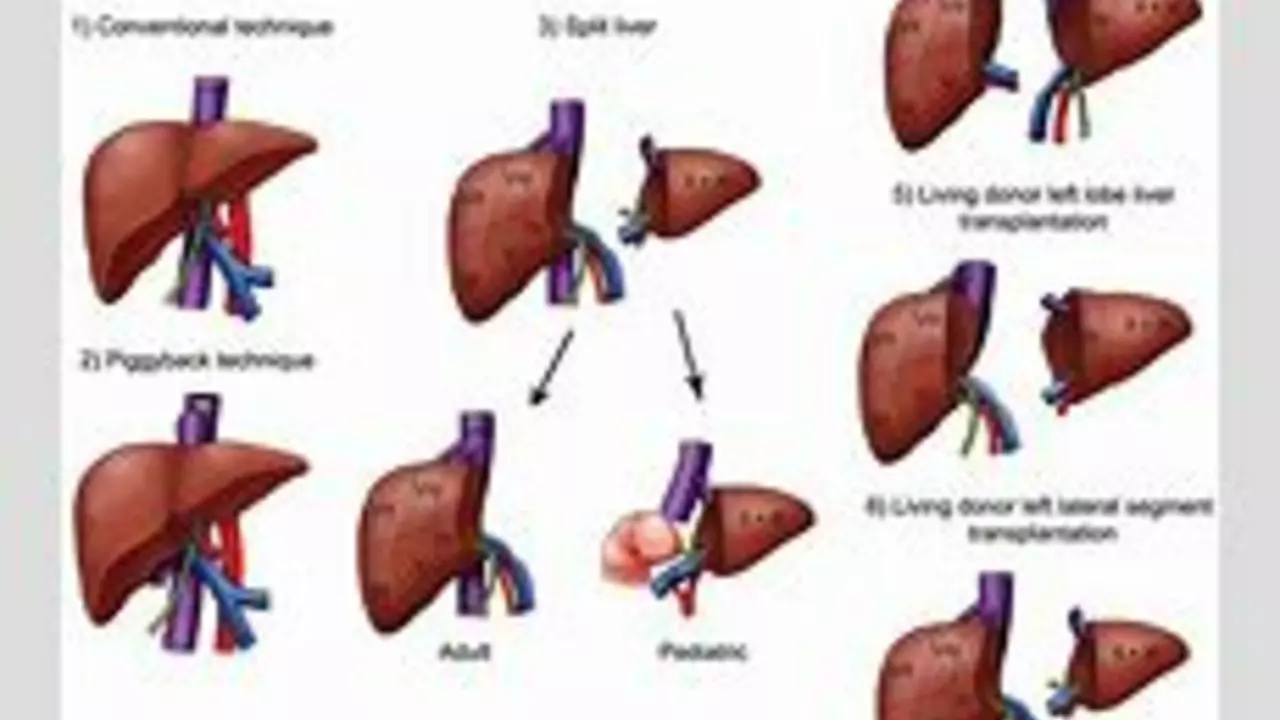
Hepatic Encephalopathy: The Role of Liver Transplantation in Treatment
Hepatic encephalopathy is a severe neurological disorder that can occur due to liver failure. In my recent research, I discovered that liver transplantation is considered the most effective treatment for this condition. The procedure helps in preventing further brain damage and improves the patient's overall quality of life. However, it's important to note that liver transplantation is a major surgery with potential risks and complications. Therefore, thorough evaluation and monitoring of patients is crucial for a successful outcome.
