What Happens When You Get Bitten?
You are hiking through tall grass in early spring. A moment later, you feel a tiny pinch on your ankle. It sounds harmless, but that small bump could be the start of something significant. This is where the story of Lyme disease begins. Unlike many infections that happen instantly, this bacterial illness follows a strict timeline. Knowing exactly how long you have before symptoms appear can change the outcome completely.
Lyme disease is a bacterial infection spread to humans through the bite of infected blacklegged ticks. First recognized in 1975 after a cluster of people developed arthritis-like symptoms in Connecticut, it remains the most reported vector-borne illness in the United States today. While you might associate it with cold winters, the bacteria causing it thrives when temperatures warm up. Understanding the progression helps you distinguish between a simple insect sting and a medical emergency.
The Culprit Behind the Rash
To understand the infection, you need to know who the enemy is. The primary cause is a spiral-shaped bacterium known as Borrelia burgdorferi. It hides inside the gut of ticks until the right conditions arrive. Not every tick carries this bacteria. Only about 10 to 30 percent of ticks found in endemic areas are actually infected. The main carrier is the blacklegged tick, or deer tick. These pests come in two main varieties depending on which side of the country you live in: the eastern Ixodes scapularis and the western Ixodes pacificus.
Transmission isn't immediate. The bacteria moves slowly from the tick's stomach to its salivary glands. Research suggests this process takes roughly 24 to 48 hours after the tick attaches. This delay gives you a window of opportunity. If you remove a tick quickly, you likely avoid infection entirely. Nymph ticks-the immature ones-are often the biggest threat because they are no bigger than a poppy seed. You won't see them easily, and that invisibility makes them dangerous during summer months when outdoor activity peaks.
| Tick Stage | Size Comparison | Risk Level |
|---|---|---|
| Nymph | Poppy seed | High (Hard to detect) |
| Adult Female | Sesame seed | Medium (Visible but common) |
Tracking the Three Stages of Progression
If the bacteria enters your bloodstream, the infection moves through three distinct phases. Each phase has a different set of symptoms and requires specific attention. Early detection is your best defense against severe complications later.
Early Localized Stage (Days to Weeks)
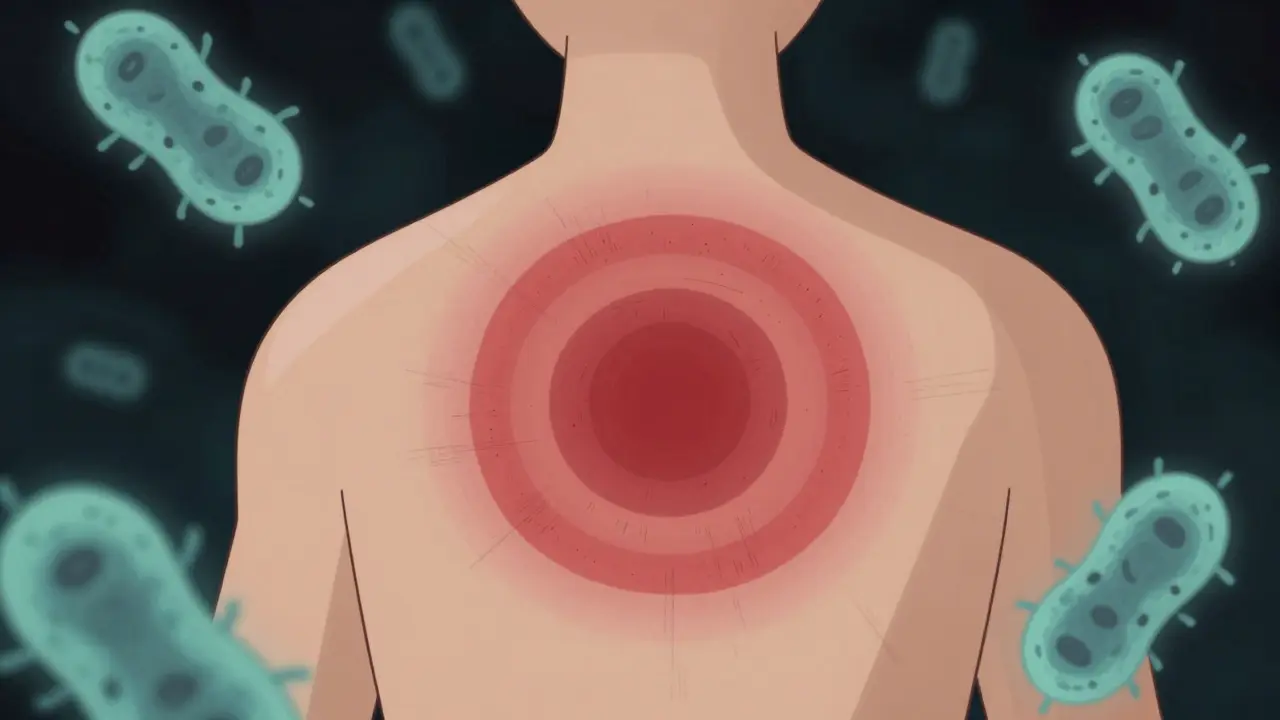
This phase happens within one month of the bite. For most people, the hallmark sign appears here: Erythema migrans. You might hear doctors call it the "bull's-eye" rash. It usually starts near the bite site and expands outward over several days. About 70 to 80 percent of patients develop this symptom. It often doesn't itch or hurt, which makes it easy to ignore. Alongside the rash, you might feel flu-like aches. Fatigue shows up in 70% of cases, headaches in 61%, and fever in nearly half of those infected. Without treatment, these symptoms fade temporarily, but the bacteria continues to travel.
Early Disseminated Stage (Weeks to Months)
Once untreated, the bacteria spreads through your blood and lymphatic system. This is where things get more serious. The single rash might multiply into several new spots on your body. Neurological signs become prominent here. Many people experience facial palsy, meaning one side of their face droops. In some cases, inflammation reaches the heart. This condition, called Lyme carditis, affects the electrical system of your heart and can cause palpitations or fainting. Joint pain might start to fluctuate in intensity. If you are diagnosed in this window, you need stronger antibiotics to halt the spread.
Late Stage (Months to Years)
Ignoring the infection past six months leads to late-stage complications. The most common issue is arthritis. Severe swelling occurs in large joints like the knees. Approximately 60% of untreated patients face this problem. Your brain may also suffer. Problems with short-term memory, concentration, or sleep patterns are frequent complaints. Chronic nerve pain and tingling sensations in extremities can occur. Once you reach this stage, recovery becomes harder and takes much longer, even with aggressive medical intervention.
Diagnosis: Why Tests Can Be Tricky
Finding out you have Lyme disease isn't always straightforward. Most standard tests look for antibodies your body creates to fight the bacteria, not the bacteria itself. This causes a major blind spot. In the early localized stage, your body hasn't produced enough antibodies yet. Standard serological testing has a sensitivity of only 29% to 40% during this phase. Doctors often rely on physical symptoms instead. The presence of the bull's-eye rash alone is considered a clinical diagnosis in many cases, according to guidelines from the Centers for Disease Control and Prevention (CDC).
Newer technology is trying to fix this gap. Direct DNA testing is emerging as a faster way to identify the pathogen earlier. In 2023, regulatory bodies approved diagnostic tools that scan urine samples for bacterial genetic material. These tests show higher sensitivity rates, potentially catching infections when antibody tests fail. Until these become standard practice everywhere, waiting for lab results means missing the best time for treatment. Always consult your physician immediately if you notice a rash after being outdoors.
Treatment Protocols and Recovery
When caught early, Lyme disease responds very well to medication. Standard protocols typically involve oral antibiotics for two to four weeks. Doxycycline is the go-to prescription for adults and children older than eight years. It is effective against the bacteria and covers other potential tick-borne diseases carried by the same tick. Amoxicillin is commonly prescribed for younger kids or pregnant women. If the infection has reached the nervous system or heart, intravenous antibiotics like ceftriaxone are necessary. The duration extends to 14 to 28 days.
Most people feel significantly better within weeks of finishing their course. However, a subset of patients reports feeling sick long after treatment ends. This phenomenon is documented as Post-Treatment Lyme Disease Syndrome (PTLDS). It affects roughly 10 to 20% of individuals. Symptoms mirror the original infection-fatigue, pain, joint issues-but the bacteria is no longer active. Experts disagree on the exact mechanism, with ongoing research investigating whether residual immune activation causes the damage rather than lingering infection. Prolonged antibiotic therapy for these persistent symptoms is controversial and generally not recommended by major infectious disease societies, though alternative management strategies are an active area of study.
Prevention Strategies That Work
Since vaccines are currently limited in availability and effectiveness, behavior remains your strongest shield. Before heading into wooded areas, wear light-colored clothing to spot ticks easier. Use EPA-approved insect repellents containing DEET or permethrin-treated gear. After returning home, shower within two hours. This washes off unattached ticks before they can embed themselves. Perform a thorough full-body check, paying close attention to hidden spots like behind ears and in hairlines.
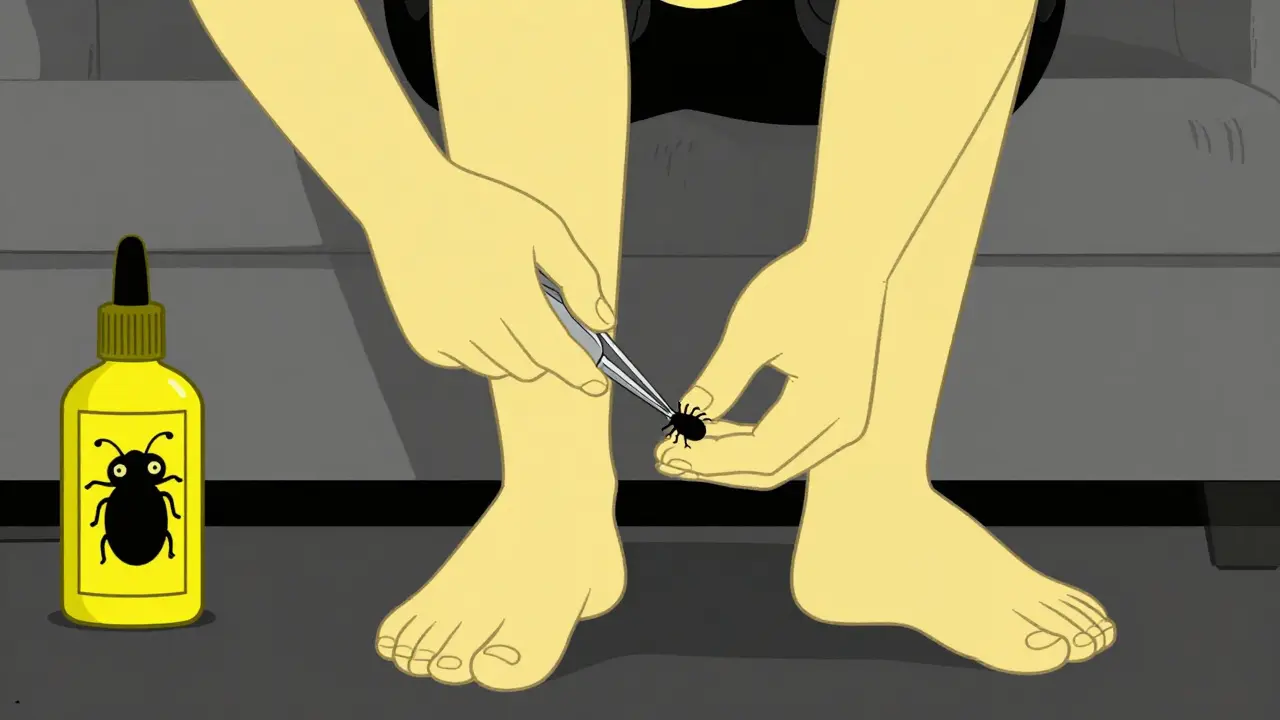
Removing a tick is simple if you have the right tools. Fine-point tweezers grip the head close to the skin. Pull upward steadily without twisting to avoid leaving mouthparts behind. Wash the area afterward. If you cannot remove the head, clean the wound and let it heal; infection from remaining parts is extremely rare compared to the risk of the initial bite. Remember that prophylactic antibiotics are sometimes used if you find an engorged tick attached for a long period, but only your doctor can prescribe this after evaluating the bite circumstances.
Living Through the Diagnosis
Navigating Lyme disease can feel overwhelming. Insurance claims data suggest hundreds of thousands of cases occur annually, yet official reporting numbers remain lower due to inconsistent testing standards across regions. Whether you suspect exposure now or years ago, early action improves odds. Stay informed about local tick activity maps. Keep communication open with your healthcare provider regarding symptoms that linger. Knowledge reduces anxiety. By understanding the timeline, you recognize warning signs sooner and advocate for yourself effectively during appointments.
How long does a tick need to stay attached to transmit Lyme?
Transmission usually requires more than 24 hours of attachment. Removing a tick within the first day significantly lowers your risk of infection.
Can you catch Lyme disease again?
Yes, reinfection is possible. Having it once does not grant immunity. Prevention steps must continue during high-risk seasons.
What is the standard treatment duration?
For early localized disease, oral antibiotics last 10 to 21 days. Disseminated or neurological cases require 14 to 28 days of intravenous medication.
Does a negative blood test rule out Lyme disease?
Not necessarily. During the first few weeks, antibody tests can produce false negatives. Clinical signs like the rash are often prioritized over lab results initially.
Are pets at risk too?
Dogs can contract Lyme disease. They act as a biological barometer-if your dog comes back with ticks, you should do a full body check immediately.


Comments
Charles Rogers
March 30, 2026 AT 00:37People truly underestimate how fast this bacteria works.
They wait too long before seeking any form of medical help.
The rash is usually right there for everyone to see clearly.
Ignoring that visual cue leads to serious trouble down the road.
Your body constantly tries to tell you something is physically wrong.
Most folks just brush the symptom off as a random bug bite.
That careless attitude puts your heart and nervous system at major risk.
Doctors eventually hate hearing about late-stage complications from patients.
Prevention is actually the most effective strategy currently available.
We need to check our skin much more often after outdoor hikes.
Showering immediately upon returning home gets rid of hidden pests.
Tweezers should definitely be in every summer survival kit at home.
Taking immediate action early saves months of unnecessary suffering later.
The timeline mentioned in this post is spot on regarding disease progression.
Nobody wants chronic arthritis caused by a tiny seed-sized bug.
Knowledge is absolute power when dealing with nature's hidden hazards.
Kendell Callaway Mooney
March 31, 2026 AT 12:25Removing the tick within twenty four hours drastically reduces infection risk.
Biraju Shah
March 31, 2026 AT 22:06The medical community has known about this for decades yet cases keep rising.
Why do we rely on tests that fail during the early phase of infection.
Clinical diagnosis using the rash should be the primary method always.
Waiting for blood work results wastes precious time.
We need stricter protocols for physicians in endemic regions.
Late stage damage is entirely preventable with early intervention.
Katie Riston
April 1, 2026 AT 13:00There is a strange beauty in how nature balances its ecosystems.Understanding this relationship changes how we approach hiking trips.
However, this balance comes at a steep cost for human visitors.
We enter these woodlands expecting peace instead of battle.
The microorganism does nothing wrong by spreading its kind.
Respect for the environment includes respecting the pathogens within it.
Knowledge turns fear into manageable caution rather than panic.
Ruth Wambui
April 2, 2026 AT 17:55They don't want you to know about the urine tests mentioned here.
Insurance companies lose money when treatments happen faster.
Standard blood panels are designed to fail early on purpose.
I suspect the bullseye rash is suppressed by big pharma protocols.
Listen to your gut feeling when doctors say wait and see.
The system is rigged against quick diagnoses for chronic conditions.
Jonathan Sanders
April 4, 2026 AT 07:05Oh look another person convinced the medical world is out to get them.
Just go to a clinic and ask for antibiotics if you have a rash.
Sometimes a problem is just a simple biological issue to fix.
Conspiracy theories dont cure joint pain or nerve inflammation effectively.
Please stop making everything sound like a grand secret design.
Brian Yap
April 4, 2026 AT 09:01Down under we deal with similar little buggers all the time mate.
You just learn to spot them before they get comfortable on you.
Australian ticks are nasty but we have good repellent options too.
The main thing is checking your dog before bringing them inside.
Cameron Redic
April 4, 2026 AT 12:07You claim transmission takes 24 hours but studies show it varies.
Some strains transfer faster under ideal temperature conditions.
Do not rely on a specific number for safety guarantees.
Statistics are averages and your body is a unique outlier sometimes.
Read the primary literature instead of summarised blog posts.
Marwood Construction
April 4, 2026 AT 23:59Safety protocols must include pre-hike inspections of clothing fabric.
Permethrin treated gear provides a necessary chemical barrier layer.
Post exposure hygiene routines are essential for field workers.
Compliance with CDC guidelines significantly lowers incidence rates.
Rick Jackson
April 5, 2026 AT 15:11Early antibiotics save lives and resources overall.
sanatan kaushik
April 6, 2026 AT 12:23Yes agreed prevention is better than cure always
dPhanen DhrubRaaj
April 8, 2026 AT 02:53i find reading the table super helpful
size comparison makes sense easily
Adryan Brown
April 9, 2026 AT 11:17It is vital that we maintain open communication with local health officials.
Reporting tick findings helps map dangerous zones for the community.
Sharing experiences supports others going through similar struggles.
Support groups exist for those facing long term recovery paths.
Persistence is required when navigating complex healthcare systems alone.
Staying calm allows you to advocate for proper diagnostic testing options.
Jonathan Alexander
April 10, 2026 AT 08:04This changed my entire weekend hiking plans completely.