Chronic Pancreatitis: What It Is and What You Can Do
Chronic pancreatitis slowly destroys the pancreas. If you keep getting upper belly pain, unexplained weight loss, or oily stools, don’t ignore it — repeated attacks can scar the gland and hurt digestion and blood sugar control. Here’s a clear, useful guide to what causes it, how doctors find it, and what you can actually do at home to feel better.
Causes & Symptoms
Most cases come from long-term alcohol use and smoking. Other causes include blocked ducts (stones or strictures), certain genetic conditions, autoimmune pancreatitis, and some medications. Symptoms vary but common ones are steady or recurring upper abdominal pain that can radiate to your back, nausea, greasy or foul-smelling stools (steatorrhea), weight loss, and new-onset diabetes.
Worried about a flare? Seek urgent care if you have severe, constant pain, fever, yellow skin or eyes, or persistent vomiting. Those signs can mean complications that need quick treatment.
Treatment & Practical Tips
Treatment focuses on three things: easing pain, fixing digestion, and treating complications. Your doctor may start with blood tests and imaging like CT, MRI/MRCP, or endoscopic ultrasound. Tests confirm damage, blocked ducts, or complications.
Simple steps you can take now: stop drinking alcohol and quit smoking — both speed up damage. Eat smaller, more frequent meals with less fat. Track what you eat and how you feel; that helps spot triggers.
Pancreatic enzyme replacement (creon-like pills) is a common and effective fix for poor digestion. Take enzymes with every meal and snack — your pharmacist or dietitian will show the right timing and dose. If you still have weight loss, ask about a high-calorie oral supplement or a feeding plan.
Pain control starts with acetaminophen or NSAIDs when possible. Some people need stronger meds, nerve blocks, or endoscopic or surgical procedures to remove blockages or relieve pressure. Discuss risks and benefits with your specialist — surgery can help some patients but isn’t needed for everyone.
Watch for diabetes. Chronic pancreatitis can damage insulin-producing cells. Get regular blood sugar checks and work with your care team to manage glucose. Bone health matters too — chronic inflammation and poor nutrition can weaken bones, so ask about vitamin D and calcium checks.
Practical support: work with a dietitian experienced in pancreatic disease, join a support group, and keep a clear list of medications and past imaging for new providers. If you’re looking for immediate relief at home, gentle walking, warm compresses, and staying hydrated can help during mild flares.
If you have ongoing symptoms or new problems, see a gastroenterologist. Chronic pancreatitis is manageable with the right plan — and small, steady changes often make the biggest difference.
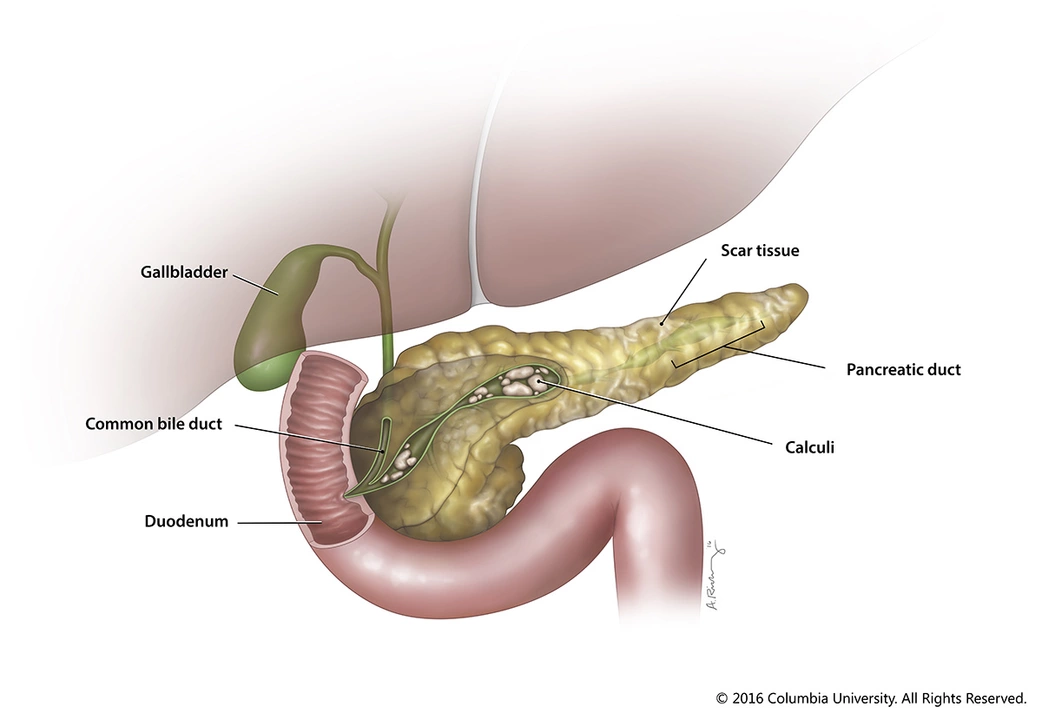
The Impact of Alcohol Consumption on Chronic Pancreatitis: Reducing Your Risk
As a blogger, I've recently delved into the topic of alcohol consumption and its impact on chronic pancreatitis. It's no secret that excessive alcohol intake can significantly increase the risk of developing this painful and debilitating condition. By reducing alcohol consumption, we can effectively lower our risk of chronic pancreatitis and improve overall health. It's crucial to spread awareness about the dangers of excessive drinking and promote healthier lifestyle choices. Remember, moderation is key, and taking care of our bodies should always be a top priority.
