Castration-resistant prostate cancer: what it means and what to do next
Castration-resistant prostate cancer (CRPC) is prostate cancer that keeps growing even when testosterone is very low. That matters because the usual hormone trick that worked before stops being enough, and your care team will change the approach. You don’t need scary jargon — you need clear steps and options. Here’s a practical guide to help you understand tests, treatments, and daily choices.
How doctors know it’s castration-resistant
Most people reach CRPC when PSA levels rise or scans show growth despite ongoing androgen-deprivation therapy (ADT). PSA can be useful but sometimes misleads, so doctors may use newer scans like PSMA PET or regular CT and bone scans to check for spread. Your team will confirm low testosterone levels first — that proves the hormone therapy is working — and then look at PSA trends, symptoms, and images to decide it's castration-resistant.
Treatment options that matter right now
There’s no single fix, but several proven choices depending on how fast the cancer is growing, where it has spread, and your general health.
- Androgen receptor (AR) pathway drugs: Enzalutamide and abiraterone block cancer’s ability to use hormones. They often work well for months to years.
- Chemotherapy: Docetaxel is a common next step when disease is aggressive; cabazitaxel can help after docetaxel stops working.
- Targeted treatments: If genetic testing shows BRCA or other DNA repair mutations, PARP inhibitors can be very effective. Ask about tumor or blood testing for these genes.
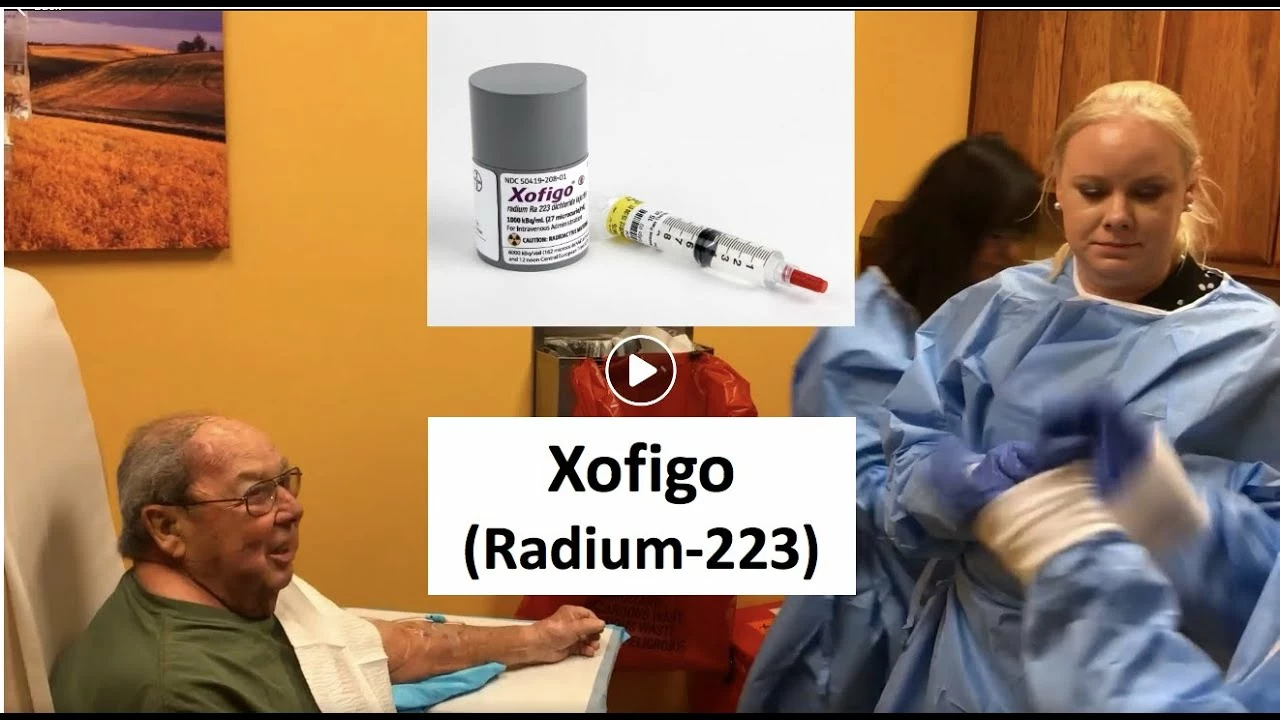
- Bone-directed therapy: If cancer reached the bones, drugs like denosumab or bisphosphonates help prevent fractures. Radium-223 is an option when bone pain and lesions are present.
- Immunotherapy and others: Sipuleucel‑T or checkpoint inhibitors may fit select patients. New drugs and combinations appear in clinical trials — often the best choice for hard-to-treat cases.
Most people move through several of these options over time. Side effects differ: hormone drugs can cause fatigue or hot flashes, chemo brings risk of infection and hair loss, and targeted drugs have their own profiles. Talk with your team about what to expect and how to manage symptoms.
Living with CRPC: practical tips
Keep a symptom log (pain, energy, appetite) and bring it to visits. Stay active — light daily exercise helps fatigue and bone strength. Ask about bone health checks and supplements like vitamin D and calcium if recommended. Control pain early with simple meds, nerve blocks, or oncology support so you stay mobile and independent.
Consider a second opinion or ask about trials if you want cutting-edge options. Genetic testing (germline and tumor) changes treatment choices for a growing number of people; it’s worth discussing. Also get support for mood, sleep, and sexual health — these affect quality of life and are treatable.
If you have questions for your doctor, ask: Why do you think it’s castration-resistant? What test should I get next? Are there trials I qualify for? What side effects should I expect and how will we manage them? Clear answers help you make practical choices every step of the way.
Flutamide in the Treatment of Non-Metastatic Castration-Resistant Prostate Cancer
As a blogger, I recently came across an interesting topic about Flutamide in the treatment of non-metastatic castration-resistant prostate cancer (nmCRPC). Flutamide is an antiandrogen medication that has shown promise in treating this specific type of prostate cancer, which is particularly challenging due to its resistance to hormone therapy. Studies have indicated that Flutamide can help slow down the progression of nmCRPC by blocking the effects of testosterone, thus inhibiting cancer cell growth. However, further research is needed to confirm its long-term efficacy and safety for patients. Overall, Flutamide seems to be a promising treatment option for those suffering from nmCRPC, and I'm excited to see what future studies reveal about its potential benefits.
