Alcohol consumption: Risks, medication interactions, and smart choices
Alcohol is part of many lives, but it’s one of the few legal substances that can change how medicines work, speed up health problems, and make recovery harder. If you take any prescription or over‑the‑counter drug, you need clear, practical advice — not scare stories. This page pulls together what matters: how alcohol affects your body, which meds clash with booze, and when to get professional help.
Alcohol and medicines: what to watch for
Mixing alcohol with medications can be harmless, risky, or downright dangerous. Some antibiotics and antivirals cause nausea or severe reactions with alcohol. Antidepressants like Tofranil (imipramine) or amitriptyline can increase drowsiness and lower coordination when combined with alcohol. Blood thinners, sedatives, and opioids raise the risk of serious bleeding, breathing problems, or overdose. If you take statins, drinking heavily can worsen liver stress and may affect sleep — see our article "Do Statins Affect Sleep?" for details on how meds and rest interact.
Medications used to treat alcohol dependence deserve special mention. Disulfiram (Antabuse) causes unpleasant reactions when you drink, while alternatives such as acamprosate take different approaches. Read "Exploring the Top 9 Alternatives to Antabuse" if you’re considering treatment options — it breaks down pros and cons without medical jargon.
Always check labels and ask a pharmacist. A simple question like “Can I drink on this medication?” can prevent hospital visits. If your doctor doesn’t bring it up, raise it yourself — it’s your safety.
Practical tips: safer use, cutting back, and spotting danger
First, know the sensible limits for your country and how a standard drink is defined. Those guidelines exist for a reason: risk rises with both amount and frequency. Second, never mix alcohol with sedating drugs, and avoid alcohol while recovering from major illness or surgery.
If you want to cut back, start with small, specific goals: skip drinks on certain days, delay your first drink, or swap to a nonalcoholic beverage at social events. Track how much you drink for a week — seeing numbers helps people change behavior fast.
Watch for warning signs that need medical attention: shakes, sweating, confusion, vomiting, racing heart, or seizures. These can be signs of severe withdrawal. If you get these, seek care right away. For milder concerns like sleep problems or drug interactions, your pharmacist or GP can usually help with safer alternatives.
Our site has related reads you might find useful: "Exploring the Top 9 Alternatives to Antabuse" for treatment choices, "Managing Sleep Issues with Ribavirin" and "Amitriptyline for Insomnia" for medication and sleep links, and practical articles on medication safety. Use them to build a clear plan before you change meds or drinking habits.
Questions for your doctor: ask how alcohol affects your specific medication, whether a short break from drinking is needed, and what signs mean you should stop drinking now. Keep the conversation simple and honest — doctors can offer realistic steps, not judgment.
Alcohol affects more than parties — it can change your medicines, your sleep, and your long-term health. Stay informed, ask questions, and get help when you need it.
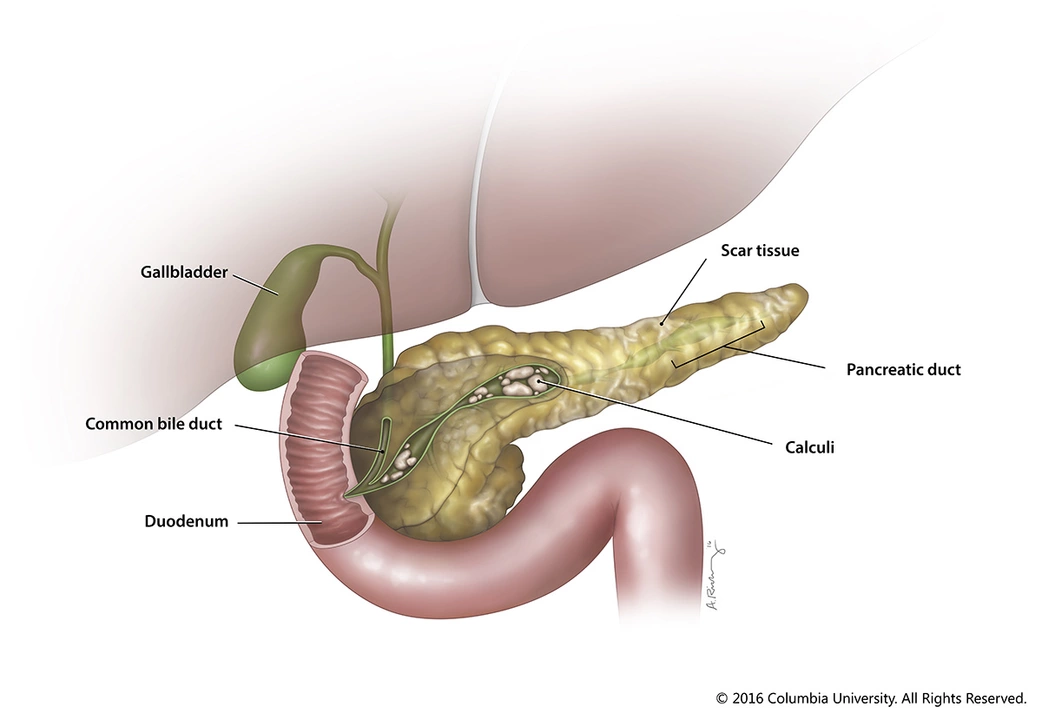
The Impact of Alcohol Consumption on Chronic Pancreatitis: Reducing Your Risk
As a blogger, I've recently delved into the topic of alcohol consumption and its impact on chronic pancreatitis. It's no secret that excessive alcohol intake can significantly increase the risk of developing this painful and debilitating condition. By reducing alcohol consumption, we can effectively lower our risk of chronic pancreatitis and improve overall health. It's crucial to spread awareness about the dangers of excessive drinking and promote healthier lifestyle choices. Remember, moderation is key, and taking care of our bodies should always be a top priority.
