When your kidneys don’t work well, your body doesn’t make enough red blood cells. This isn’t just about feeling tired-it’s a serious medical issue called anemia in kidney disease. About 90% of people with advanced kidney failure develop this condition. The reason? Damaged kidneys stop producing erythropoietin, the hormone that tells your bone marrow to make red blood cells. But that’s only half the story. Iron, which your body needs to build those cells, also gets stuck and unusable. Treating this isn’t as simple as taking an iron pill. It’s a careful balance of hormones, iron doses, and constant monitoring.
Why Anemia Happens in Kidney Disease
Chronic kidney disease (CKD) slowly damages the tiny cells in your kidneys that produce erythropoietin. By the time someone reaches stage 4 or 5 CKD, they’re making less than 10% of the erythropoietin they used to. Without it, your bone marrow doesn’t get the signal to make red blood cells. That’s why hemoglobin-a protein in red blood cells that carries oxygen-drops below normal levels. For men, that’s under 13 g/dL; for women, under 12 g/dL.
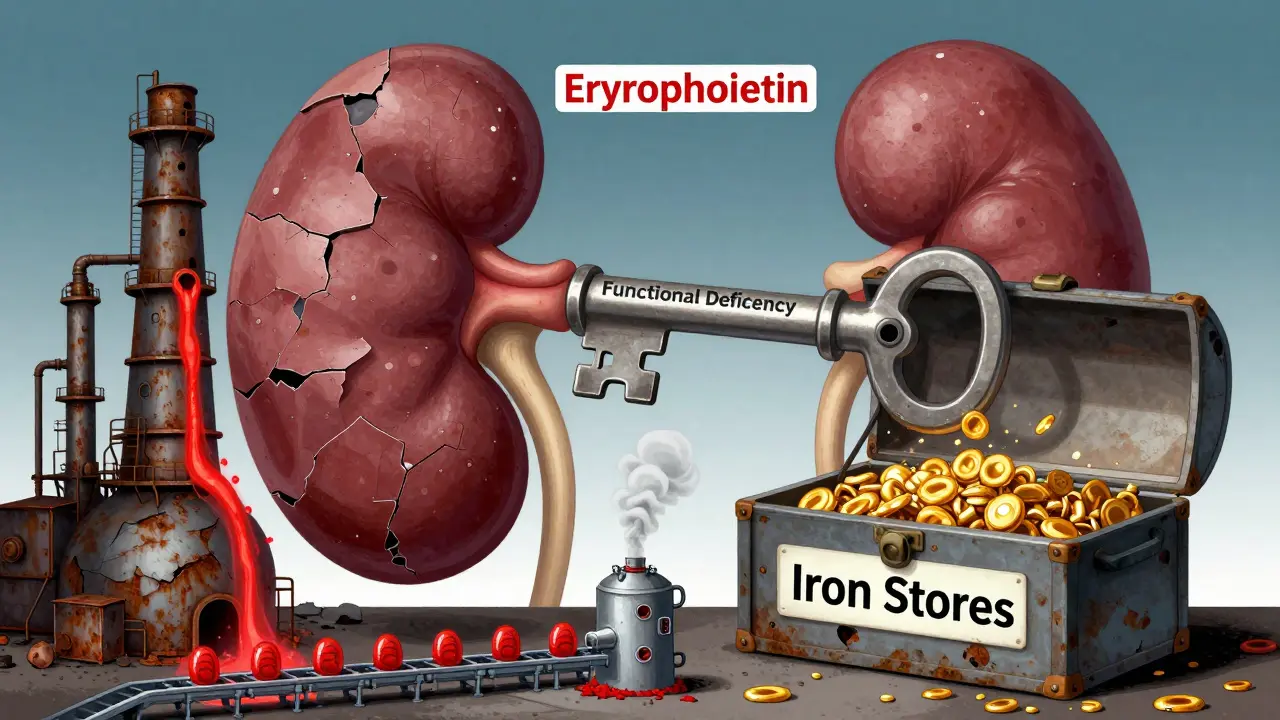
But here’s what most people miss: even if you have enough iron in your body, it can’t get to where it’s needed. Inflammation from kidney disease triggers a hormone called hepcidin, which acts like a lock on iron stores. Iron stays trapped in your liver and spleen, not in your bloodstream. That’s called functional iron deficiency. You might have plenty of iron, but your body can’t use it. That’s why oral iron pills often fail in CKD patients-only 30-40% gets absorbed, compared to nearly 100% with intravenous iron.
Erythropoiesis-Stimulating Agents (ESAs): The Hormone Replacement
Recombinant human erythropoietin, first approved in 1989, changed everything. Drugs like epoetin alfa, darbepoetin alfa, and biosimilars like Retacrit now replace what your kidneys can’t make. These are given either under the skin (subcutaneous) for non-dialysis patients or through an IV during dialysis. Dosing varies: epoetin alfa at 200-10,000 units, darbepoetin alfa at 0.45 mcg/kg weekly. They typically raise hemoglobin by 1-2 g/dL in 2-6 weeks.
But ESAs aren’t magic bullets. If your iron is low, they won’t work. That’s called ESA hyporesponsiveness. About 10% of CKD patients don’t respond because their iron isn’t fixed first. And if you push hemoglobin too high-above 11.5 g/dL-you increase stroke risk. The TREAT trial in 2009 showed a 32% higher stroke rate when doctors targeted 13 g/dL instead of 9-11 g/dL. That’s why current guidelines, like KDIGO’s 2025 draft, say: aim for 10-11.5 g/dL. Not higher. Not lower. Just right.
Iron Therapy: The Missing Piece
Oral iron? Often useless. Iron pills get blocked by hepcidin, cause nausea, and rarely improve hemoglobin in CKD. Intravenous iron is the gold standard. Iron sucrose (Venofer), ferric carboxymaltose, and other IV forms bypass the gut and deliver iron directly into the bloodstream.
When should you start? KDIGO’s 2025 draft says: if ferritin is below 500 mcg/L and transferrin saturation (TSAT) is under 30%. For hemodialysis patients, many experts give 400 mg of IV iron monthly-whether they’re deficient or not. Why? Because inflammation makes iron levels unreliable. It’s preventative, not reactive.
IV iron works fast. A 1,000 mg total dose can lift hemoglobin by 1.5 g/dL in just four weeks. But it’s not without risks. About 45% of patients report a metallic taste after infusion. 28% feel flu-like symptoms. Rarely, severe allergic reactions happen-about 1 in 500 doses. And if ferritin climbs above 800 mcg/L, you risk iron overload, which can damage your heart and liver.

The New Frontier: HIF-PHIs
For years, ESAs and IV iron were the only tools. Now, oral drugs called HIF-PHIs (hypoxia-inducible factor prolyl hydroxylase inhibitors) are changing the game. Roxadustat, approved in the U.S. in December 2023, and daprodustat work differently. Instead of replacing erythropoietin, they trick your body into making more of it naturally. They also improve iron use by lowering hepcidin.
This means better iron availability without needing IV iron as often. In trials, roxadustat raised hemoglobin as well as ESAs-but with fewer cardiovascular events in some subgroups. It’s taken orally, so no injections. For patients who hate needles or have trouble getting to dialysis, this is huge.
But there’s a catch. Early studies raised red flags about tumor growth in cancer patients. The FDA placed clinical holds between 2018 and 2020. Now, after more data, it’s approved-but only for CKD patients without active cancer. Long-term safety is still being studied.
How Treatment Really Works: The Step-by-Step Process
There’s no guessing in this treatment. It follows a clear path:
- Confirm anemia. Check hemoglobin, mean corpuscular volume (MCV), and reticulocyte count. Rule out other causes like bleeding or vitamin B12 deficiency.
- Check iron status. Measure ferritin and TSAT. If ferritin is below 100 mcg/L, you have absolute iron deficiency. If ferritin is 100-500 and TSAT is below 20-30%, you have functional deficiency. Both need IV iron.
- Start IV iron. For hemodialysis patients, give 400 mg monthly. For non-dialysis, give 200-400 mg weekly until ferritin reaches 500-700 mcg/L and TSAT is over 30%.
- Start ESA if needed. Only if hemoglobin stays under 10 g/dL after iron repletion. Begin with low doses and adjust slowly.
- Monitor monthly. Hemoglobin should rise no more than 1 g/dL per month. Too fast? Risk of clots. Too slow? You’re not helping.
Doctors who follow this exactly see fewer transfusions, less hospitalization, and better energy levels. Patient forums like DaVita’s show 68% report being able to play with grandchildren or walk without getting winded within four weeks.

What Goes Wrong? Common Pitfalls
Even with clear guidelines, mistakes happen.
- Over-treating hemoglobin. Keeping it above 11.5 g/dL increases stroke risk. Yet, 22% of U.S. dialysis patients still have levels above 11 g/dL.
- Ignoring iron. Giving ESA without fixing iron first leads to hyporesponsiveness. The patient keeps getting higher doses, but hemoglobin doesn’t budge.
- Using oral iron. It’s cheap, but ineffective in CKD. It doesn’t fix the hepcidin block. You’re wasting time and money.
- Not checking ferritin. A normal ferritin doesn’t mean enough iron is available. Inflammation can mask true deficiency.
One Mayo Clinic case from 2022 showed a 62-year-old diabetic patient whose hemoglobin jumped from 8.2 to 10.5 g/dL in eight weeks-after switching from oral iron to IV iron and starting darbepoetin. He went from needing naps after walking to the mailbox to gardening again.
What’s Next? The Future of Treatment
The market for anemia treatments in CKD was $12.8 billion in 2022. ESAs still make up 75% of sales. But HIF-PHIs are growing fast. Roxadustat and daprodustat could hit $3.5 billion in sales by 2028.
Research is moving toward personalization. Mayo Clinic is testing machine learning to predict the exact ESA dose a patient needs, cutting dose variability by 22%. Minihepcidins-tiny molecules that block hepcidin-are in early trials. They could free up iron without needing IV iron at all.
One thing’s clear: the one-size-fits-all approach is over. Dr. Iain Macdougall of King’s College Hospital said it best: “Targeting a single hemoglobin number for everyone is outdated and potentially harmful.” Today’s goal isn’t just to raise numbers. It’s to help people feel better, stay out of the hospital, and live longer-with fewer side effects.
Can anemia in kidney disease be cured?
No, not permanently. Anemia in kidney disease is caused by kidney damage, which can’t be reversed in most cases. But it can be controlled. With the right combination of iron therapy and erythropoiesis-stimulating agents (or HIF-PHIs), most patients can maintain hemoglobin in the safe range of 10-11.5 g/dL and feel much better. A kidney transplant can restore normal erythropoietin production and cure the anemia-but that’s not an option for everyone.
Why not just take iron pills for kidney anemia?
Oral iron rarely works in kidney disease. Inflammation triggers hepcidin, a hormone that blocks iron absorption in the gut and traps iron in storage organs. Studies show only 30-40% of oral iron is absorbed, compared to nearly 100% with IV iron. Plus, oral iron causes nausea, constipation, and stomach pain in 40% of users. IV iron skips the gut entirely, delivers iron directly into the bloodstream, and works faster with fewer side effects.
What’s the best hemoglobin target for someone with kidney disease?
The current guideline from KDIGO (2025 draft) recommends keeping hemoglobin between 10 and 11.5 g/dL. Going above 11.5 g/dL increases the risk of stroke, heart attack, and blood clots. Going below 10 g/dL leads to fatigue, shortness of breath, and reduced quality of life. The goal isn’t to hit a number-it’s to match the patient’s symptoms. Someone who feels fine at 10.2 g/dL doesn’t need to be pushed higher.
Are HIF-PHIs better than ESAs?
For many patients, yes. HIF-PHIs like roxadustat are taken orally, improve iron use by lowering hepcidin, and may carry lower cardiovascular risks than high-dose ESAs. They’re especially helpful for patients who dislike injections or have trouble with IV access. But they’re not for everyone. They’re not approved for patients with active cancer due to potential tumor growth risks. ESAs are still the first choice for most, but HIF-PHIs are becoming a strong alternative.
How often do you need IV iron?
For hemodialysis patients, most guidelines recommend 400 mg of IV iron every month. But it depends on your ferritin and TSAT levels. If ferritin is above 700 mcg/L or TSAT is over 40%, you may pause iron until levels drop. For non-dialysis patients, doses are smaller-200-400 mg weekly-until iron stores are replenished. Monitoring every 1-3 months is key. Too little iron, and ESA won’t work. Too much, and you risk organ damage.

Comments
trudale hampton
March 22, 2026 AT 18:21Really solid breakdown. I’ve been managing CKD for 5 years now, and this is the first time I’ve seen the hepcidin-iron trap explained so clearly. IV iron was a game-changer for me - no more 3 p.m. naps. I didn’t even know my body was hoarding iron like a dragon with a gold hoard.
Shaun Wakashige
March 24, 2026 AT 11:16lol at the 10-11.5 g/dL target. they really think we’re all on a diet or something 😅
Jackie Tucker
March 26, 2026 AT 00:16How quaint. We’ve been treating anemia with hormones and IV iron since the 90s - as if the body were a broken vending machine. Meanwhile, the real issue is systemic inflammation, which no one wants to talk about because it doesn’t sell drugs. HIF-PHIs? Just another profit-driven rebrand. The body doesn’t need ‘tricking’ - it needs healing. But sure, let’s keep monetizing the symptoms.
Thomas Jensen
March 26, 2026 AT 18:55Wait - so if you’re on dialysis and they give you IV iron every month… what if that’s just to keep you dependent? What if the real reason they don’t fix kidneys is because the anemia treatment is a $12 BILLION industry? I mean, think about it. Kidney transplants cure it. But they don’t do them unless you’re rich. Coincidence? I think not.
matthew runcie
March 27, 2026 AT 04:28Iron and EPO together work. Simple. No drama. Just follow the steps. I’ve seen it save people’s lives.
shannon kozee
March 27, 2026 AT 06:47Oral iron doesn’t work because of hepcidin. IV iron bypasses it. That’s the whole point. No need to overcomplicate.
Paul Cuccurullo
March 28, 2026 AT 09:44It’s truly remarkable how far we’ve come. From patients gasping for air on the couch… to walking their dogs, playing with grandchildren, feeling human again. This isn’t just medicine - it’s dignity restored. Every dose of IV iron, every ESA adjustment - it’s not just numbers. It’s a return to life.
Solomon Kindie
March 29, 2026 AT 18:57hif phis are just a temp fix like everything else. they lower hepcidin but dont fix the kidney damage. its like putting duct tape on a ruptured pipe. the body still cant make erythropoietin. and what about the cancer risk? they say 'no active cancer' but what about latent? no one talks about that. also i think they just want to sell more pills. its always pills. never cure. just manage.
Natali Shevchenko
March 31, 2026 AT 13:30It’s fascinating how the body’s response to low oxygen isn’t just about replacing one hormone - it’s an entire adaptive cascade. HIF-PHIs don’t just stimulate erythropoietin; they rewire the metabolic environment. Lower hepcidin, increase iron mobilization, enhance oxygen delivery efficiency - it’s like the body finally gets to use its own ancient survival mechanisms instead of relying on synthetic replacements. We’re not just treating anemia anymore. We’re participating in a physiological reawakening. It’s almost poetic, if you think about it - the body remembering how to breathe, even when its kidneys have forgotten.
Nicole James
April 2, 2026 AT 03:55Wait… so they’re giving IV iron EVERY MONTH… even if ferritin is high?? And they call it ‘preventative’? That’s not preventative - that’s reckless. What if someone has hemochromatosis? What if they’re absorbing iron from supplements? What if the lab is wrong? And why isn’t anyone asking about the long-term liver damage? Who’s monitoring this? Who’s auditing the hospitals? I’ve seen people with ferritin over 1000 - and they’re still getting IV iron. This isn’t medicine - it’s industrial routine.
Desiree LaPointe
April 3, 2026 AT 01:22Oh wow, a 12.8 billion dollar industry? And we’re all just supposed to be grateful that they’re ‘helping’ us with IV drips and injections? How charming. Let me guess - the same people who profit from ESAs also fund the KDIGO guidelines? And the ‘clinical holds’ on HIF-PHIs? Just a little hiccup before the FDA rubber-stamped it. Please. We’re not patients - we’re revenue streams with pulse rates.